'My mole is very dark, is that normal?' is one of the most common questions a consultant dermatologist hears. The honest answer is that darkness on its own is rarely the deciding feature. Plenty of entirely benign moles are very dark brown or black. A small minority of melanomas are amelanotic and contain almost no pigment at all. The colour itself is less important than the pattern, the uniformity, and the stability over time.
What separates a dark benign mole from a dark melanoma is mostly visible to a trained eye with dermatoscopy and only partially visible to the naked eye. This guide walks through the visual features that an adult can reasonably assess at home, the limits of that assessment, and the dermatoscopic features that the consultant will look for when self-assessment runs out.
Written and medically reviewed by a GMC-registered consultant plastic surgeon who performs melanoma excisions weekly and reads thousands of dermatoscopic images a year.
Why darkness alone isn't the issue
Many of the moles that visually 'pop' against pale skin and cause patients to book a consultation are entirely benign compound naevi. They're dark because the melanocyte cluster sits relatively superficially and the surrounding skin is light. The clinical conversation usually ends with reassurance: yes it's a striking mole, no it doesn't have any concerning features, no action needed.
Conversely, some of the most aggressive melanomas are pale or skin-coloured. Amelanotic melanomas account for about 5% of melanoma cases and contain so little pigment that they fail every colour-based ABCDE feature.[1] They appear pink, red, or skin-coloured, and are routinely missed by self-checking that focuses on darkness.
The takeaway. Darkness is one variable, not the variable. The features that actually distinguish benign from malignant in pigmented lesions are uniformity within the lesion (one shade vs multiple), symmetry of shape and colour distribution, border quality, size, and most importantly change over time. A uniformly dark mole that's been the same for ten years is reassuring. A previously pale mole that's developed a dark patch over six months is not.
What you can reasonably assess to the naked eye
The ABCDE framework, covered in detail in our standalone guide, is the right starting point for a dark mole. Asymmetry: do the two halves of the mole look the same when imagined folded in half? Border: is the edge clean and consistent or notched/scalloped/fading? Colour: a single shade of dark brown is reassuring; multiple shades layered (black plus brown plus red, or pale patches inside a dark area) are not. Diameter: above 6mm warrants a closer look, below 6mm doesn't automatically reassure. Evolving: change in any feature over weeks or months is the strongest single warning.
For dark moles specifically, two ABCDE features carry extra weight. Asymmetric darkness within the lesion (one half meaningfully darker than the other, or a focal dark spot inside an otherwise mid-toned mole) is a stronger flag than uniform darkness. Borders that fade outward into surrounding skin (rather than stopping cleanly) suggest pigment has spread peripherally, which is more characteristic of melanoma than of benign moles.
What you cannot reliably assess to the naked eye are the dermatoscopic features that distinguish benign and malignant pigment networks: pigment streaks, atypical reticular patterns, blue-white veil, regression structures. These are visible only under the polarised dermatoscope and require pattern-recognition training. This is why even a confident self-assessment of a dark mole has a meaningful error rate; the consultant assessment is the actual diagnosis.[2]
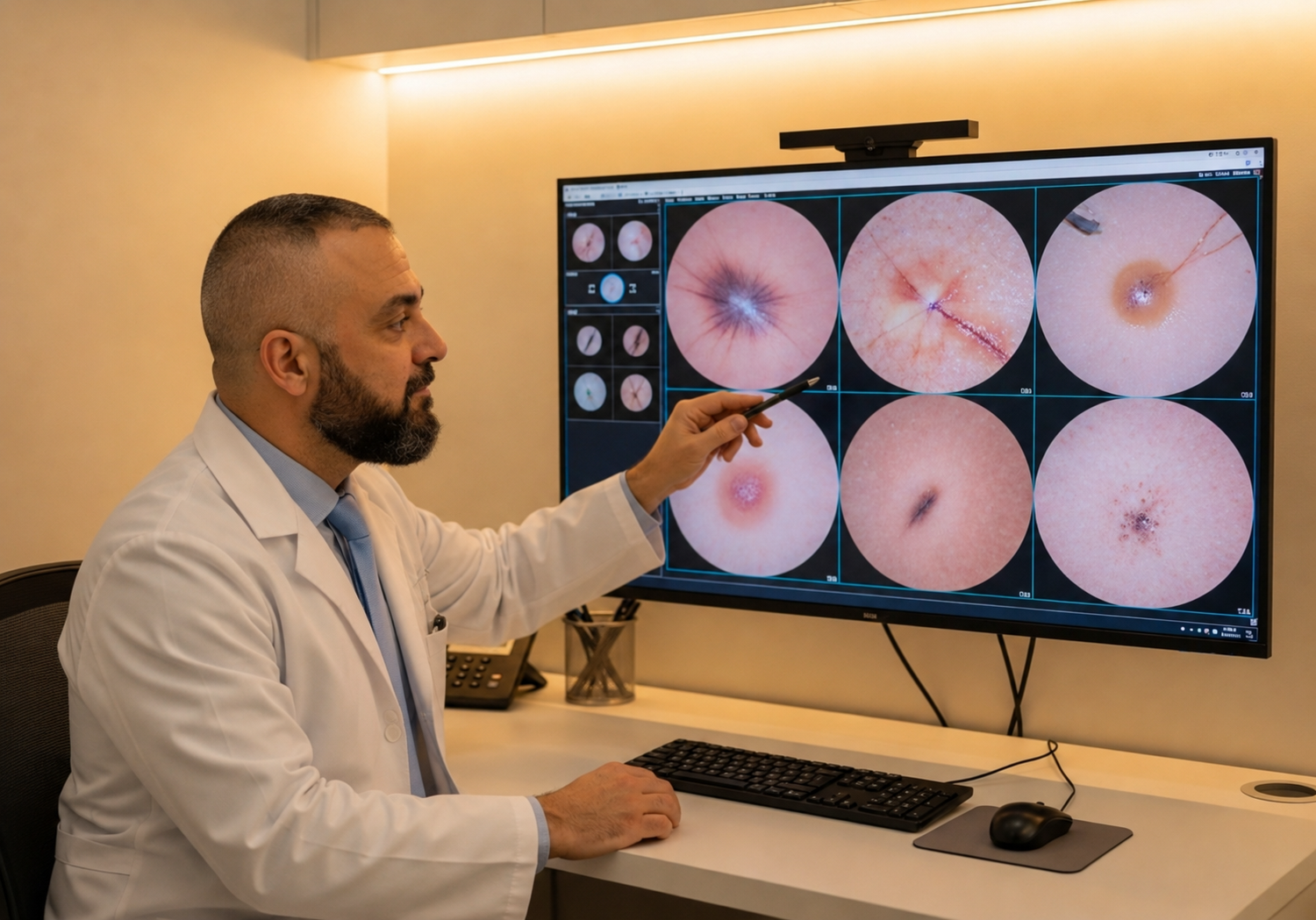
What dermatoscopy adds
Dermatoscopy is high-magnification examination with a polarised light source that eliminates surface reflection. It allows the consultant to see structures sitting in the upper dermis that are invisible under normal viewing conditions: pigment networks, vascular patterns, dot and globule patterns, and structural symmetry across multiple axes.
For dark moles specifically, dermatoscopy resolves three questions the naked eye cannot. Is the dark pigment epidermal or deeper? Surface pigment in benign moles produces a regular brown reticular network; deep pigment in melanoma produces irregular blue-grey or blue-black structures (the 'blue-white veil') that signal melanocytes invading the dermis. Is the pigment distributed evenly? Benign dark moles show pigment evenly across all four quadrants of the dermatoscopic view; melanomas show asymmetric distribution often confined to one or two quadrants. Is there active change? Atypical pigment networks at the lesion's periphery, irregular streaks, or regression structures (white scar-like areas) suggest active progression.
The diagnostic accuracy of expert dermatoscopy is meaningfully higher than naked-eye examination alone, particularly for dark lesions where the colour can be visually arresting without being clinically significant. A 2008 meta-analysis showed dermatoscopy plus expert eye outperforms expert eye alone for melanoma detection across multiple settings.[3]
Common dark benign moles you'll see
Three benign categories account for most of the dark moles patients worry about. Compound naevi are the most common adult mole type, with melanocytes spanning the dermo-epidermal junction and the upper dermis. They can be quite dark, are usually 4-6mm, slightly raised, with a soft texture and clean border. Patients hearing 'compound' from their consultant should hear it as reassurance.
Blue naevi are small, dome-shaped, and surprisingly blue or blue-grey to the naked eye because their melanocytes sit deep in the dermis and the depth shifts the perceived colour through skin overlying them. They are usually under 5mm, well-circumscribed, and entirely benign. The unusual colour can be alarming, but dermatoscopy resolves it quickly.
Spitz naevi typically appear in children and adolescents as fast-growing, pink or reddish dome-shaped lesions, but pigmented variants exist that can be very dark. Histologically they share features with melanoma, and even experienced dermatopathologists sometimes find them difficult to distinguish, so excision and histology are commonly recommended even when the lesion is most likely benign. The combination of rapid growth + dark colour + young patient is the typical presentation.
What dark melanomas actually look like
Most cutaneous melanomas in the UK are of the superficial spreading subtype: a flat, asymmetric pigmented patch that grows laterally for years before becoming invasive. Visually, they're typically 6mm+, asymmetric, with multiple shades of brown plus often a darker central area or peripheral black streaks. The border is irregular, often notched. Most patients notice them because they look different from the rest of their moles, not because they look dramatically dark on their own.
Nodular melanoma is the more aggressive subtype, a raised dome-shaped lesion that grows vertically (into the dermis) without the long lateral phase. It can be very dark, smooth-surfaced, often without classical ABCDE features, and tends to develop quickly over weeks to months. The EFG framework (Elevated, Firm, Growing) is more useful for nodular detection than ABCDE.[4]
Lentigo maligna is a slow-growing form of melanoma in situ that prefers chronically sun-damaged skin (face, scalp, ears, dorsum of hands, lower legs). It presents as an irregular brown-to-dark patch that grows slowly across years, often mistaken for a sun-spot or seborrhoeic keratosis. After age 60, any new pigmented patch on chronically sun-exposed skin deserves a consultant assessment, including for lentigo maligna.
Practical self-check rules for dark moles
Apply these in order. First, take a dated photograph of the dark mole today. Whatever you decide next, having a baseline image makes the future easier. Second, compare with your other moles. Is this dark mole strikingly different in shade or pattern from your other moles, or does it broadly fit your usual pigmentation? Strikingly different is a flag.
Third, apply ABCDE strictly. Does the dark mole show asymmetry, irregular border, multiple colours within it (not just being uniformly dark), diameter over 6mm, or evolving features? Any single feature warrants a consultant; two or more warrants one within a week.
Fourth, consider age and location. A dark mole in your twenties on your back is different from a dark mole on your face in your sixties. Location matters: chronically sun-exposed sites in older adults have a higher prior probability of skin cancer. Fifth, trust your instinct. Patients are often right when something feels wrong, even when they can't articulate exactly why. If you keep returning to that one mole in the mirror, book the consultation.
When to act, and what we'll do
Book within a week if any of: the dark mole has visibly changed in 1-3 months; it's bleeding, crusting, or persistently itching; it shows two or more ABCDE features; it's strikingly different from your other moles; it's new in adulthood, particularly after age 50.
Book within a month if a single ABCDE feature is present without recent change, or if you'd simply like reassurance and a documented baseline. The £250 mole check covers consultation, dermatoscopy, written report within 24 hours, and any same-day excision with histology if indicated.
What we do at the appointment: structured clinical history, naked-eye examination of the dark mole plus surrounding skin, dermatoscopy with the consultant's screen turned to face you so you can follow the reasoning. Findings discussed in plain language, with one of three outcomes: reassure (no action, ongoing self-monitoring), monitor (re-photograph at 3-6 months), or excise with histology (full-thickness elliptical excision under local anaesthetic, sent to a UKAS-accredited lab, results within 7-10 working days). Most dark moles are reassured; the minority that need excision usually have it the same day.
Common questions
Frequently asked
References
Sources cited
- McClain SE, Mayo KB, Shada AL, et al. Amelanotic melanomas presenting as red skin lesions: a diagnostic challenge with potentially lethal consequences. Int J Dermatol. 2012;51(4):420-426. View source
- Argenziano G, Soyer HP, Chimenti S, et al. Dermoscopy of pigmented skin lesions: results of a consensus meeting via the Internet. J Am Acad Dermatol. 2003;48(5):679-693. View source
- Vestergaard ME, Macaskill P, Holt PE, Menzies SW. Dermoscopy compared with naked eye examination for the diagnosis of primary melanoma. Br J Dermatol. 2008;159(3):669-676. View source
- Kelly JW, Chamberlain AJ, Staples MP, McAvoy B. Nodular melanoma: no longer as simple as ABC. Aust Fam Physician. 2003;32(9):706-709.
- British Association of Dermatologists. Guidance on the management of melanoma. 2021 update. View source